CLEVELAND — A young Cleveland couple recently faced a frightening situation with their first pregnancy. They got the care they needed, but ended up with a confusing and costly medical bill.
Dec. 7 of last year won’t be forgotten by Kevin Sloan.
“It was probably the scariest day of my life,” said Sloan. His wife was 22-weeks pregnant at the time with their first child, but she was in severe pain.
They rushed to the closest emergency room, which was Cleveland Clinic’s Fairview Hospital.
"We had been there before, actually, and it had been covered by our insurance,” Sloan told us.
He said the wife’s ovary had been twisted and she had surgery right away.
"(The doctors said) if we had waited longer, might have had to remove the ovary or part of it, might have been really bad for the pregnancy,” Sloan told us.
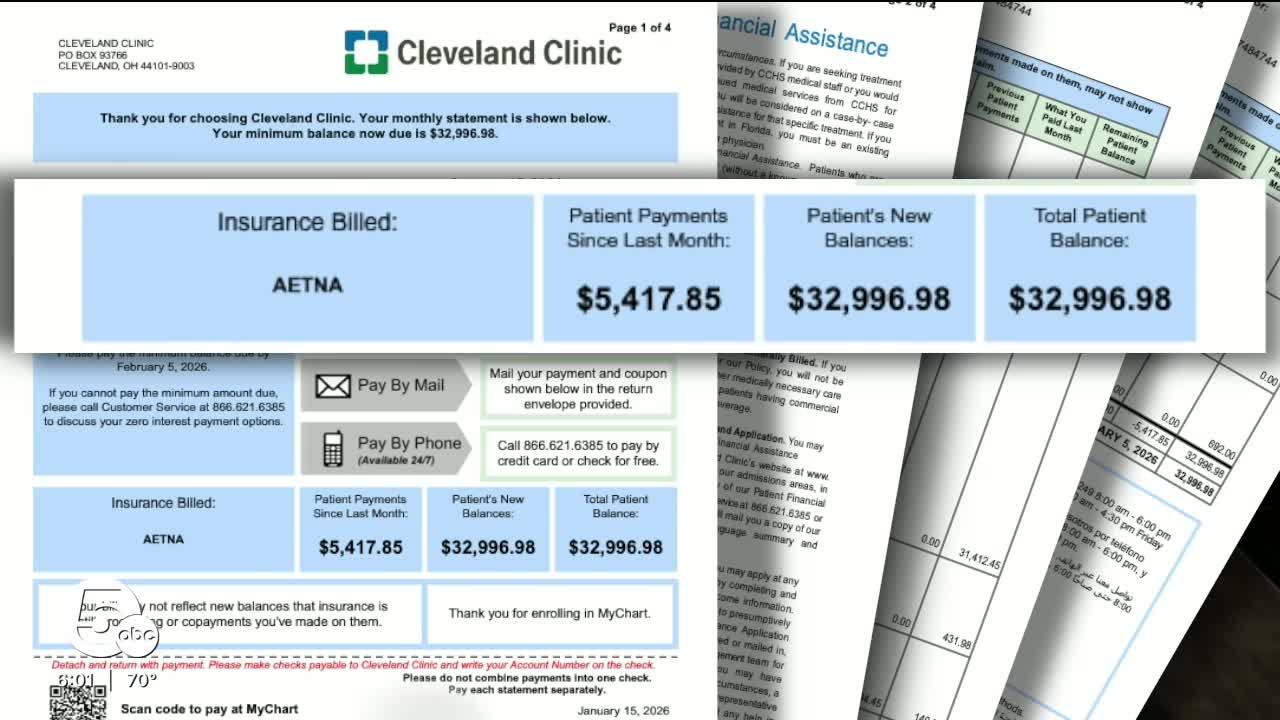
He said he was grateful for the medical care that day. Baby and mom are fine, but he was not grateful for the $32,000 bill that claimed the surgery was elective and out-of-network.
Sloan told us he battled the bill with Cleveland Clinic and his insurance company, Aetna, but was denied again and again.
"My reaction was this is so obviously a mistake,” said Sloan.
At The Gathering Place in Beachwood, Eileen Coan helps cancer patients with their billing. She said, in general, you shouldn’t pay the first bill, but don’t ignore them either. She suggested asking for an itemized bill because you can find mistakes.
"They’ll say I didn’t get a scan on that day or I never met that doctor,” said Coan about what she hears from the people she helps.
She encouraged people to push their doctors’ offices, keep asking them questions.
"Have you tried again? Have you resubmitted it? Is there a different code that you can use? Can you argue my case? Yes, this is a new drug, but it is the only drug we think might help me,” said Coan.
And keep in mind, pharmaceutical businesses are required to help lower-income people.
"By law, every drug company has to have a compassionate care program,” Coan told us.
She told us that on the back of every bill, there’s information about payment plans. She said you should set up one and make sure every doctor and facility billing you is put into the same payment plan pot.
For Sloan, he contacted the News 5 Investigators. We started asking Cleveland Clinic and Aetna questions. They then reviewed the couple’s case and now insurance told us it “should not have been processed as out-of-network, and aetna will cover the appropriate charges….” (full statement below)
"Know what your rights are,” said Sloan. “And if people authoritatively tell you your rights are not your rights, don’t believe them.”
This story came to us from Sloan reaching out. We can help you, too. Email us at InvestigatorTips@WEWS.com or call our tip line at 216-431-4357 (HELP).
Aetna Statement:
“We are dedicated to ensuring the best possible experiences and outcomes for our members, and we appreciate when concerns are brought to our attention. After further review, we determined that this case should not have been processed as out-of-network, and Aetna will cover the appropriate charges. We are also taking steps to review and enhance our administrative processes to make it as easy as possible for members to access their benefits.”